Adding genetics to a patient's clinical profile might lead to more accurate blood-thinner dosing
Including genetic information in a patient's clinical profile might help determine the optimal starting dose of the common blood-thinner Warfarin, according to findings from a large-scale study that will be published in the New England Journal of medicine.
Researchers from more than 20 scientific teams in nine countries on four continents collaborated on the project. Stanford University helped coordinate the study. The findings are described in the article, "Warfarin Dosing Using Clinical and Pharmacogenetic Data."
Warfarin is often prescribed to prevent blood clots in people with certain heart conditions or other serious diseases. Getting the right starting dose can be tricky because people vary in their responses to the drug. A patient taking too high a dose may begin bleeding. If the dose is too low, deadly blood clots might form. The safest, most effective dose can vary by a factor of 10 among different patients.
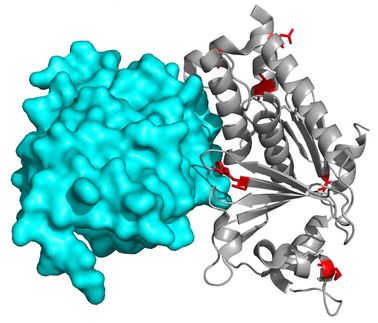
In 2002 and again in 2005, University of Washington (UW) pharmacy and genome science researchers made major contributions in the field of genetic variations that influence how an individual responds to warfarin. David Veenstra of the UW School of Pharmacy and his colleagues found that patients with genetic variants in the human enzyme that metabolizes warfarin required lower doses and were more likely to suffer bleeding problems from the drug.
Later, Allan E. Rettie, professor and chair of medicinal chemistry in the UW School of Pharmacy, Mark Rieder, research professor of genome sciences in the UW School of Medicine, and their colleagues showed that warfarin response can also be affected by variations in the gene encoding vitamin K epoxide reductase (VKORCI). Retrospective studies suggested that variations in this gene stratified patients into low-dose, intermediate dose, and high-dose warfarin groups.
Their work helped set the stage for future research on what is often called personalized medicine, in which a person's genetic makeup might be used to individualize and optimize drug therapy. Veenstra, Rettie, Rieder and Lisa Meckley, also of the UW School of Pharmacy, contributed data and helped in the interpretation of the data analysis for the study being published in tomorrow's New England Journal of Medicine.
The Consortium combined anonymous clinical and genetic data from 5,052 patients taking warfarin. They created two dosing algorithms: one with only clinical variables, such as height, weight, diabetes and other conditions, and additional medications taken, and another using both clinical variables and genetics, which they called the pharmacogenetic algorithm. They compared these algorithms with each other and with a fixed-dose strategy, and then compared the algorithm-derived dose estimates with the dosages actually received by patients.
They found that the pharmacogenetic model was significantly better than both the clinical algorithm and the fixed dosage strategy in predicting starting dosages that were closer to the required stable therapy warfarin dose, especially for those patients in the low-dose or high-dose groups. The pharmacogenetic algorithm was less likely to overestimate the dose for the low dose group, or underestimate the dose in high dose group.
Most read news
Other news from the department science

Get the analytics and lab tech industry in your inbox
By submitting this form you agree that LUMITOS AG will send you the newsletter(s) selected above by email. Your data will not be passed on to third parties. Your data will be stored and processed in accordance with our data protection regulations. LUMITOS may contact you by email for the purpose of advertising or market and opinion surveys. You can revoke your consent at any time without giving reasons to LUMITOS AG, Ernst-Augustin-Str. 2, 12489 Berlin, Germany or by e-mail at revoke@lumitos.com with effect for the future. In addition, each email contains a link to unsubscribe from the corresponding newsletter.